
SARS 2002: How a Chinese Farmer Sparked a Global Crisis
The 2002 SARS outbreak, starting with a Chinese farmer's fever, exposed critical flaws in global health security. Learn how to prevent the next pandemic.
The unseen threat: Our global health defense
On November 16, 2002, a Chinese farmer got a fever and a cough. Doctors in Guangdong quickly found a cluster of similar cases. They faced an unknown respiratory illness. This quiet start began the Severe Acute Respiratory Syndrome (SARS) outbreak. It showed how fast a local threat could become a global crisis.
Global health security protects people from infectious disease outbreaks. It means stopping, finding, and fighting health threats that cross borders. Threats can come from animals, labs, or people. The World Health Organization (WHO), national agencies like the U.S. Centers for Disease Control and Prevention (CDC), and NGOs such as Doctors Without Borders (MSF) are important organizations. We live in an interconnected world. Fast travel and trade make every local outbreak a possible global emergency. Weak health systems in one country threaten everyone.
SARS: We weren’t ready
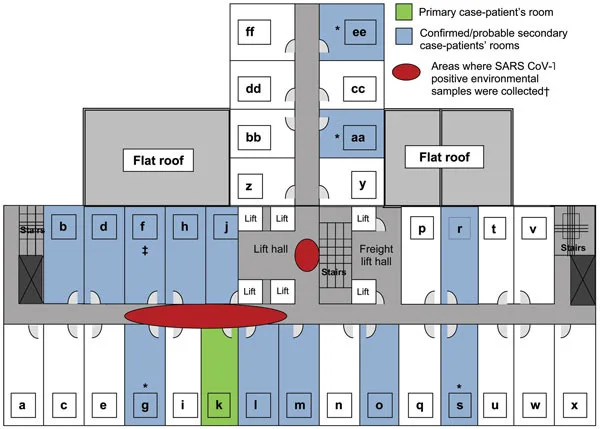
SARS spread fast beyond Foshan. On February 21, 2003, a doctor from Guangdong went to Hong Kong. He stayed at the Metropole Hotel. He unknowingly infected guests from Singapore, Vietnam, and Canada. This one event turned a regional problem into a worldwide concern. Within weeks, SARS hit 30 countries.
The world reacted slowly and without coordination. Countries shared little information. Nations restricted travel without clear guidance. The economic damage was huge. The World Bank estimated SARS cost the global economy between $30 billion and $50 billion. This financial toll showed we urgently needed better international cooperation.
SARS was a tough lesson. Dr. David Heymann, then WHO’s communicable diseases head, said the world had “dodged a bullet.” The experience prompted a big change in international health law. On May 23, 2005, the World Health Assembly adopted the revised International Health Regulations (IHR). These regulations became a legally binding agreement. Countries would use them to stop, find, assess, and respond to public health risks. Their goal was to stop disease spread globally. They also aimed to limit disruption to travel and trade.
The Metropole Hotel in Hong Kong became an unwitting epicenter of the SARS outbreak in 2003. A single infected doctor staying here unknowingly transmitted the virus to guests from multiple countries, dramatically accelerating its global spread. (Source: commons.wikimedia.org)
H1N1: The framework’s first test
The revised IHR took effect in June 2007. They required all 196 signatory countries to build basic capabilities: surveillance systems, lab diagnostics, and emergency response plans. Nations had until 2012 to meet them. But many countries had trouble meeting these.
On April 11, 2009, the WHO confirmed the first human case of a new influenza A (H1N1) virus in Mexico. The virus spread fast. On June 11, 2009, WHO Director-General Dr. Margaret Chan declared H1N1 a pandemic. This was the first global influenza pandemic in 41 years. The world now faced a new test for its health security.
H1N1 showed progress, but also ongoing problems. The IHR allowed faster information sharing than during SARS. Scientists quickly identified the virus. Vaccines developed quickly. By late 2009, pharmaceutical companies had produced millions of vaccine shots.
Still, many countries faced challenges. Some didn’t have enough vaccine supplies. Others struggled to distribute them. Public health systems were strained. A 2011 WHO report found many nations still hadn’t met IHR basic capability requirements. This left gaps in the world’s defense against future outbreaks.
Ebola: A new push for security
In March 2014, Guinea confirmed an Ebola outbreak. It then spread fast into Liberia and Sierra Leone. This West African Ebola epidemic became the largest ever. It showed serious weaknesses in health systems and global response. The world’s initial reaction was slow and disorganized.
Local health workers, often without enough protection, faced the main impact of the crisis. Doctors Without Borders (MSF) played an important role. They set up treatment centers. They documented the emergency’s huge size. Dr. Joanne Liu, then International President of MSF, warned the UN Security Council that the world was “losing the battle” against Ebola. The virus infected over 28,000 people and killed more than 11,000.
Ebola’s devastating impact led to new global health security efforts. In February 2014, before Ebola’s full size hit, the U.S. launched the Global Health Security Agenda (GHSA). This initiative brought together nations, international organizations, and civil society partners. Its goal was to help countries meet IHR rules faster. GHSA focused on clear, measurable goals. These covered 11 action areas, like biosafety, surveillance, and emergency operations.
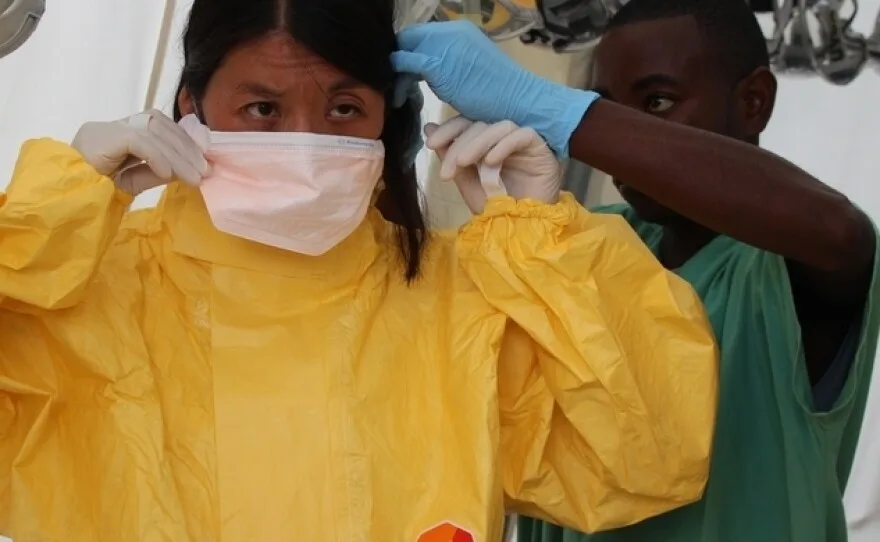
During the devastating 2014-2016 West African Ebola epidemic, organizations like Doctors Without Borders (MSF) established critical treatment centers. These facilities, often staffed by healthcare workers in full protective gear, were at the forefront of the crisis, providing care and highlighting the urgent need for global health security improvements. (Source: kpbs.org)
Ebola also led the World Bank to create the Pandemic Emergency Financing Facility (PEF) in 2017. This fund provided quick funding for low-income countries facing outbreaks. These efforts showed the world was more dedicated to readiness. But the next major pandemic would show how much more work was needed.
COVID-19: The world wasn’t ready
On December 31, 2019, China reported a cluster of unknown pneumonia cases in Wuhan. Within weeks, a new coronavirus, SARS-CoV-2, began its fast global spread. On January 30, 2020, WHO Director-General Dr. Tedros Adhanom Ghebreyesus declared the outbreak a Public Health Emergency of International Concern (PHEIC). This was the most serious alert level under the IHR.
COVID-19 quickly became a pandemic. It infected and killed millions worldwide. The virus strained healthcare systems. It harmed economies and interrupted daily life in new ways. Many countries, despite years of warnings, were unprepared. Supply chains for PPE and medical supplies broke down. Rapid testing and contact tracing efforts often failed.
The pandemic showed clear unfairness. Rich countries quickly got vaccine doses. Low-income nations waited months or even years. The COVAX Facility, meant to ensure fair vaccine distribution, faced difficulties. Dr. Tedros often spoke out against “vaccine nationalism.” He called for more global solidarity. A 2021 report by the Independent Panel for Pandemic Preparedness and Response (IPPPR) found the world “unprepared and uncoordinated” for COVID-19. The IHR, despite its purpose, failed to stop a terrible global health crisis.
Rebuilding trust, reinforcing defenses
After COVID-19, the world saw a strong need for stronger, fairer global health security. In December 2021, the World Health Assembly agreed to begin negotiations for a new international instrument. This proposed Pandemic Agreement seeks to improve global cooperation and preparedness. Discussions are happening. They focus on fair access to vaccines, data sharing, and stronger governance.
Other initiatives have started. The World Bank started a new Pandemic Fund in September 2022. This fund provides money for pandemic prevention, preparedness, and response (PPR) in low- and middle-income countries. It aims to address the serious lack of investment that contributed to the COVID-19 disaster. The G7 and G20 groups also pledged to strengthen global health security. They stress the “One Health” approach. This recognizes the connection between human, animal, and environmental health.

The COVAX Facility was established to ensure equitable access to COVID-19 vaccines globally, especially for low-income countries. Despite its crucial mission, it faced significant challenges including 'vaccine nationalism' and supply chain issues, highlighting global disparities in pandemic response. (Source: cepi.net)
These efforts urge us to learn from past failures. They want to make sure no country is left behind when the next disease appears. But lasting political will and sufficient funding are vital. Without these, even the best plans might fail.
Questions you might have
How does climate change affect health security? Climate change changes disease patterns. It expands vector habitats and increases extreme weather. It creates new health risks, displaces people, and strains health systems. This makes global health security efforts more complex and urgent.
What is the Pandemic Agreement? The Pandemic Agreement is a proposed international treaty. WHO member states are negotiating it. It aims to strengthen global preparedness and response for future pandemics. Key goals include fair access to medical tools and better surveillance.
The path ahead: shared responsibility
We repeatedly learn tough lessons in global health, often too late. SARS, H1N1, Ebola, COVID-19 – each crisis revealed our weaknesses. Each also prompted us to build stronger defenses. The next disease will surely come, not if, but when. New diseases, drug-resistant germs, and climate change all present growing dangers.
True global health security needs more than just new treaties or funds. It needs ongoing investment in strong national health systems. It means building trust and openness between nations. It also needs fair access to tools, treatments, and vaccines. One nation’s health is directly linked to everyone’s. This shared responsibility is our only way forward. It’s time we truly accepted it.

Extreme weather events, exacerbated by climate change, directly threaten global health security by displacing populations, damaging infrastructure, and creating conditions ripe for disease outbreaks, as seen in communities recovering from devastating floods or prolonged droughts. (Source: eea.europa.eu)
You might also like:
👉 Significant Medical Breakthroughs: A Journey Through Medicine History
👉 Virtual Reality in Healthcare: Revolutionizing Medicine & Patient Care
👉 Unexplained Mysteries of Science: Cosmos, Quantum & Beyond
